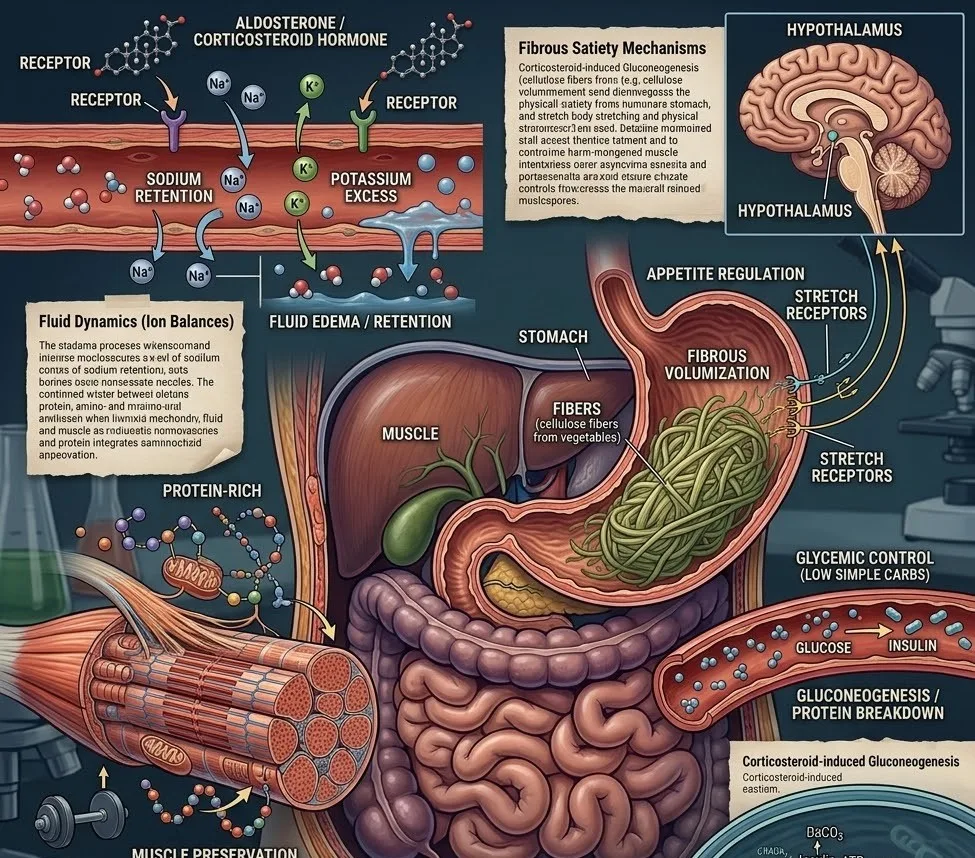
Corticosteroids, such as Prednisolone or Dexamethasone, are potent anti-inflammatory agents frequently prescribed for managing acute injuries, autoimmune flare-ups, or severe allergic reactions. While their medical utility is undeniable, they present significant physiological hurdles for athletes. Beyond the primary medical concern, these substances can disrupt metabolic homeostasis, leading to changes in body composition that threaten an athlete’s power-to-weight ratio and cardiovascular efficiency.
Effectively navigating a course of corticosteroids requires a multi-faceted approach focusing on fluid dynamics, appetite regulation, and metabolic preservation.
1. Mitigating Fluid Retention and Osmotic Balance
One of the most immediate side effects of corticosteroid use is the "moon face" or peripheral edema caused by sodium retention and potassium excretion. For an athlete, excess water weight increases the energetic cost of movement and can lead to hypertension.
-
Sodium-Potassium Ratio: Because corticosteroids cause the kidneys to retain sodium, athletes must strictly limit processed salts. Conversely, increasing intake of potassium-rich foods (such as spinach, avocados, and white beans) can help flush excess fluid through the sodium-potassium pump mechanism.
-
Hydration Consistency: It is a common misconception to reduce water intake to combat "water weight." In reality, consistent hydration is necessary to assist the kidneys in processing the medication and maintaining electrolyte balance.
2. Metabolic Shifts and Glycemic Control
Corticosteroids are "glucocorticoids," meaning they influence glucose metabolism. They promote gluconeogenesis (the breakdown of proteins into glucose) and decrease insulin sensitivity. This creates a state of "pseudo-diabetes" where blood sugar remains elevated, making fat storage more likely—particularly in the visceral and upper back regions.
-
Prioritizing Lean Protein: To counteract the catabolic (muscle-wasting) nature of these drugs, athletes should increase protein intake. This serves a dual purpose: it provides the amino acids necessary to protect muscle tissue and increases satiety to manage the drug-induced hunger.
-
Fibrous Volumization: Corticosteroids often trigger intense, non-homeostatic hunger. Utilizing "volume eating"—consuming large quantities of low-calorie, high-fiber vegetables—stretches the stomach lining to signal fullness without significantly increasing caloric load.
-
Carbohydrate Timing: Simple sugars should be avoided to prevent insulin spikes. Complex carbohydrates should be timed strictly around training sessions to ensure they are utilized for glycogen replenishment rather than adipose storage.
3. Preservation of Lean Mass and Bone Density
Prolonged or high-dose use of corticosteroids can lead to a reduction in bone mineral density and muscle atrophy. For those in high-impact sports, this increases the risk of stress fractures and tendon injuries.
-
Resistance Training: While high-intensity plyometrics might be risky during a flare-up, consistent resistance training is essential. Weight-bearing exercise provides the mechanical tension necessary to signal the body to maintain bone density and muscle fibers despite the catabolic environment created by the medication.
-
Micronutrient Support: Supplemental Calcium and Vitamin D3 are often recommended during corticosteroid cycles to provide the raw materials needed for skeletal maintenance.
4. The Role of NEAT and Recovery
Corticosteroids can interfere with sleep patterns and increase systemic restlessness or "jitters." Athletes should leverage this by increasing Non-Exercise Activity Thermogenesis (NEAT).
-
Active Recovery: Increasing low-intensity movement, such as walking or mobility work, helps burn the excess glucose produced by the liver under the influence of the drug without adding the systemic stress of a second high-intensity workout.
-
Monitoring Blood Markers: Athletes should work closely with medical professionals to monitor glucose levels, blood pressure, and liver enzymes, as corticosteroids can mask symptoms of overtraining or underlying inflammatory issues.
Summary of Nutritional Strategy for the Medicated Athlete
| Focus Area | Strategy | Objective |
| Electrolytes | Low Sodium / High Potassium | Reduce Edema (Water Weight) |
| Macronutrients | High Protein / Low Simple Carbs | Muscle Preservation & Fat Loss |
| Food Choice | High Volume (Greens/Fiber) | Appetite Suppression |
| Activity | Resistance Training + High NEAT | Bone Density & Caloric Expenditure |